What can orthotics do for me?
Orthotics can provide pain relief and ongoing health benefits for people suffering from:
- Plantar fasciitis
- Heel and arch pain
- Achilles tendon pain
- Fallen arches
- Low arches
- High arches
- Rheumatoid and osteoarthritis
- Lower back pain
- Knee pain
- Hip pain
- Knocked-knees
- Bowed legs
- Ball of foot pain
- Morton’s neuroma
- Bunions and big toe joint pain
- Lateral column overload
- Cerebral palsy
- Ankle pain
- And much more

What are the different types of orthotics?
At Entire Podiatry we offer our patients three different types of orthotics. We offer these different options to ensure that there is an affordable treatment option to suit your needs and budget.
- Custom foot orthotics
- Semi-customised foot orthotics or CFAs
- Minimally customised or professional ‘Off-the-Shelf’ orthotics
Your podiatrist will be able to talk to you in detail about which of these three orthotic options will be best suited to you.
Custom foot orthotics
A customised foot orthotic provides the best and most advanced means of correcting and controlling your foot function. This is the most effective type of orthotic to address pain in your feet, ankles, knees, hips and lower back.
Based on studies it has been shown that the most effective custom orthotics are made using state-of-the-art 3D scanning technology. At Entire Podiatry a 3D scan is taken of your foot; this scan perfectly captures the shape and size of your foot and will capture any individual ‘quirks’ of your feet. This degree of customisation allows the orthotic to conform perfectly against your foot to ensure the pressure is spread evenly across the entire surface of the foot. A study in 2002 compared two foot imaging techniques and it showed that non-weight bearing foot imaging was the most reliable method for making custom orthotics.1
Do not get confused by some podiatrists who use a 3-D pressure map of the foot as this unfortunately is not the best technique to capture the image. Patients in this instance are asked to walk across a force plate and a pressure map is produced on the computer. This method does not accurately capture the correct shape of the foot and subsequently the orthotics that are produced are inferior.
Once the 3-D scan is taken at Entire Podiatry the orthotic is then manufactured. The orthotic is designed and built in a specific way based on your ‘prescription’. Similar to an optical prescription, no two people’s custom orthotic prescription will be the same. Your podiatrist develops your prescription after they have assessed your feet and gait based on your clinic needs.
The result is a perfectly customised orthotic device created from your exact foot shape and your precise mechanics to give the best biomechanical correction and comfort.
Article citation:
1 A comparison of four methods of obtaining a negative impression of the foot. McClay-Davis I, Laughton C, Williams, DS. J Am Podiatr Med Assoc. 2002 May;92(5):261-8
Semi-customised orthotics or CFA (Cast and Foot Adjusted) orthotics
Cast and Foot Adjusted (CFA) orthotics offer a lower cost alternative to custom orthotics. While CFA orthotics incorporate an element of individual modification, they are less precisely matched to your individual foot than custom foot orthotics.
CFA orthotics are made from a library of standard foot moulds/shapes. The standard foot mould that matches your foot most closely will be used to manufacture your orthotics. This is determined after your podiatrist has taken an outline of your feet, and conducted a biomechanical assessment to prescribe the type of correction your feet require.
There are many options for the type of orthotic shell used within the range of CFA orthotics, which enables this to be matched as closely as possible to your foot type. However, if you have a unique foot type, such as very flat feet, high arched feet, wide or narrow feet, then CFA orthotics are unlikely to be a suitable option for you. CFA orthotics are made based on a closely matched indication of foot type, but they do not detect discrete, unique specifications of your feet. As such, we don’t expect CFA orthotics to achieve the same level of improvement in foot function as custom orthotics, but in some cases they are a worthwhile option.
Minimally customised orthotics or off-the-shelf professional orthotics
Minimally customised orthotics or professional OTS (off-the-shelf) orthotics are another option that Entire Podiatry offer our patients. These devices are a lower-cost option but have a lesser element of customisation. There is a range of OTS orthotics for both adults and children.
It’s important to note that not everyone may be suited to this range of orthotics. For example if you have a very high arch or a very flat foot, you will likely not be suited to this type of orthotic. If you are planning on wearing the orthotics into dress shoes, football boots or sandals then this type of orthotic is also less likely to be suitable as these orthotics are typically bulkier and we are unable to modify them to compliment certain shoes. If you have a particular pain or symptom which requires a certain type of biomechanical correction to resolve, then these OTS orthotics may offer insufficient correction and you may find more benefit from an orthotic with a higher degree of customisation in order to address your requirements.
What are my orthotics made from?
A lot has changed over the past few years in the orthotic manufacturing industry. There are now more orthotic material options than ever. Entire Podiatry pride ourselves on keeping up with the latest advances and ensuring we offer a range of different orthotic materials to suit your needs.
Orthotic materials that are ideal for one individual could be detrimental to another. This is why your individual foot requires individual attention.
The type of material used is based on factors such as:
- Your symptoms
- Your foot type and foot shape
- The types of shoes the orthotics are going to be worn in
- Activities you’ll be doing when wearing the orthotics
- Your body weight
- The amount of correction required to improve your foot function
- Your preferences

You may have heard the term ‘rigid foot orthotics’. These orthotics are typically made from a plastic such as polypropelyne or subortholene. Don’t be put off by the term ‘rigid’ used to describe these orthotics. The shells can be made from flexible, semi-flexible, semi-rigid or rigid materials and your podiatrist can dictate the amount of rigidity required in their prescription.
Recently, new developments in orthotic manufacturing and material creation have led to the development of new carbon orthotics. These orthotics are made from carbon fibre and are the most ultra-lightweight and thin devices on the market. Carbon fibre orthotics are perfect for fitting into tighter footwear that may have difficulty accommodating a traditional orthotic.
At Entire Podiatry we also manufacture our orthotics from a foam/rubber material called EVA (Ethyl Vinyl Acetate). The EVA material comes also comes in three different densities depending on the patient’s requirements. EVA orthotics have great cushioning effects and are very easily modified or adjusted. A popular option for those who require a very cushioned custom soft foot orthotic is low-density EVA. This material is incredibly soft and cushioned beneath the foot, perfect for those with sensitive feet or with painful conditions beneath the feet that require lots of cushioning.
After the material of the shell has been chosen, most orthotics are made with an additional layer of material over the top of the device. This acts as a cover and increases the longevity of the orthotic and provides cushioning. We have numerous different types of cover materials depending on your needs and preferences. For example, we have a natural leather orthotic material that is perfect for those with allergies to synthetic materials. We have extra absorbent and quick drying material perfect for those prone to sweaty feet. We also have a range of bright and fun colours and patterns for kids to choose from.
Other types of orthotics you may have heard of
Gel orthotics
Gel orthotics can be purchased from the chemist or supermarket and claim to fix many different foot problems.
“People may receive a small amount of benefit from such purchases, but they usually find their pain is not resolved adequately.” – Chris Hope, Podiatrist
This is because these gel innersoles fail to provide adequate support and are not correcting biomechanical abnormalities. This is because the gel ‘orthotics’ purchased from the chemist are a ‘one size fit all’ approach. Whilst they provide some additional cushioning beneath the foot they do not take into consideration how much support is required for your specific foot and your specific pain, injury or requirement.
Original copper heeler orthotics
Original Copper Heeler Orthotics are a brand of insoles which claim to relieve pain from arthritis. The copper is said to be absorbed through the skin and circulates through the body to reduce joint discomfort. There has been no scientific studies and no evidence to support this claim. It could simply be the fact that these orthotics support the arch and this support reduces the arthritis pain rather than the effect of the copper, or the effects could be a placebo. Either way, further research needs to be undertaken to support their claim and most modern podiatry clinics do not support these or manufacture their orthotics from copper materials.
Orthotics & foot pain
Orthotics for Achilles tendon pain
Achilles tendinopathy is a painful condition which affects the back of the heel at the Achilles tendon. The pain may occur in the tendon, or the pain may be lower at the back of the heel bone, where the tendon attaches to the heel. (Click here for more information on Achilles Tendinopathy). Typically the pain begins during or after exercise or when you stand up and get moving after while of being off your feet. If the condition is left untreated then the pain can be present almost constantly.
Treatment for Achilles tendinopathy includes a combination of rest, pain relief, changes to footwear, stretches/strengthening and often orthotics.
Most people receive benefit from a pair of orthotics for Achilles tendonitis treatment. Improper foot function or poor foot mechanics is a lead cause of Achilles Tendinopathy. For example, a foot that rolls in or pronates excessively, or a foot with a very rigid and high arch can cause the Achilles tendon to be overloaded.
The best orthotics for Achilles tendonitis is a device which conforms well through your foot and is designed in such a way to reduce the strain going through your overloaded Achilles. Orthotics for Achilles tendonitis can provide a rapid reduction in symptoms, can encourage the tendon to heal and can reduce the likelihood of the problem reoccurring.
Can orthotics cause Achilles pain?
At Entire Podiatry we have sometimes been asked “can orthotics cause Achilles pain?”. We believe that orthotics can be incredibly useful, but if they are not prescribed correctly they may cause discomfort. When prescribed properly however, by a qualified podiatrist, orthotics can be highly valuable to the wearer.
A study in 2014 observed the effect of using orthotics on the Achilles tendon. They found that running with foot orthotics resulted in a reduction in Achilles tendon load compared to running without orthotics. This study suggest that foot orthotics significantly reduce the stress on the Achilles tendon in runners.1
“A study…found that running with foot orthotics resulted in a reduction in Achilles tendon load compared to running without orthotics”
When prescribed unnecessarily or incorrectly, orthotics can be unsafe and may aggravate an underlying pre-existing medical condition. People at particular risk are those with Achilles tendon pain, heel pain, knee or back problems, or those who have flat feet or a high arch foot type. So it is important to obtain professionally fitted orthotics. If you are experiencing pain in your heels or any of the aforementioned pain, contact us at Entire Podiatry today. We can help determine the best solutions to reduce your pain.

Article citation:
1 Sinclair J, Isherwood J, Taylor P. Effects of foot orthoses on Achilles tendon load in recreational runners. Clinical Biomechanics. 2014;29(8):956-958.
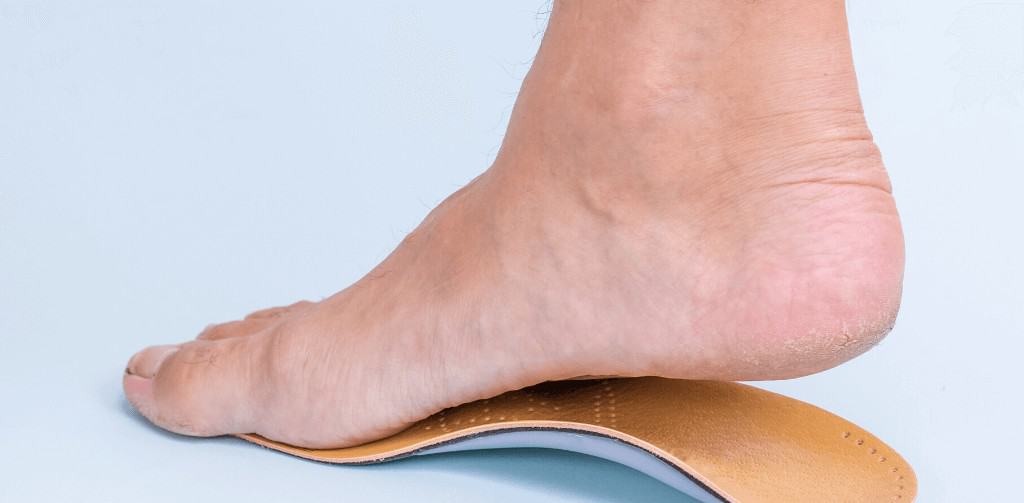
Orthotics for flat feet and medial arch support
Many people have flat feet, where the feet tend to roll in and the arch of the foot drops to the ground (otherwise known as fallen arches). While this is a common foot type, lacking a natural arch in the foot can place strain on surrounding soft tissues, and the biomechanics associated with a flat foot type can lead to pain through the feet, ankles, knees, hips or even the lower back.
Not everyone who has flat feet will experience symptoms. But for some people, particularly those who enjoy an active lifestyle, having flat feet can be problematic and unnecessarily limiting.
There are a range of different treatment options for people with flat feet, one of which is orthotics. But while many of us have heard of orthotics before, you may be unsure of how orthotics can help with flat feet.
How do orthotics help with flat feet?
Orthotics optimise the position and alignment of the feet to improve posture, stability and foot function. In the case of flat feet, where the feet have a tendency to roll in, orthotics support the arch of the foot to reduce excessive weight-bearing forces on the inside of the feet. This promotes a more natural curve in the arches of the feet and reduces strain being placed on surrounding muscles, ligaments and tendons.
There are a few different types of orthotics available on the market, each offering varying levels of support. Total Contact Orthotics, which are custom-made to suit an individual’s foot, generally are the best orthotics for arch support and the best orthotics for fallen arches.
As the name implies, Total Contact Orthotics are designed to offer a high level of contact between the sole of the foot and the orthotic. This is best achieved through a process of conducting a comprehensive biomechanical assessment and taking a scan of the feet, following which the podiatrist writes a script so that orthotics are made in accordance with the podiatrist’s specifications.
Do I need orthotics for fallen arches or flat feet?
Not all flat feet will require orthotics, and depending on the cause of your symptoms, other treatment methods can also provide relief. For example, supportive footwear (with or without orthotics) and specific stretching and strengthening exercises, may assist to minimise symptoms associated with flat feet. However, many people with flat feet do experience improved comfort and symptom relief from orthotics for arch pain, heel pain, generalised foot pain, and pain in the ankles, knees and legs. A full length pair of foot arch orthotics can be manufactured specifically for those individuals seeking additional support and comfort.
If you have a very low arch, we recommend custom foot orthotics. A customised low arch orthotic will ensure the appropriate amount of support, without irritating the foot, and provide an arch fill to create your perfect arch orthotics. The amount of fill used when making an arch fill orthotic is a specific criteria that a podiatrist uses to determine how much support is given to the patient’s foot.
There are many studies which have shown how orthotics are beneficial for people with flat feet. For specific advice and individual assessment of your flat feet, make an appointment to see one of our podiatrists at Entire Podiatry. 123
Article citations:
1 Noll K. The use of orthotic devices in adult acquired flatfoot deformity. Foot and Ankle Clinics. 2001;6(1):25-36.
2 Michelson J, Durant D, McFarland E. The Injury Risk Associated with Pes Planus in Athletes. Foot & Ankle International. 2002;23(7):629-633.
3 Parsons S. Correction and prevention of deformity in type II tibialis posterior dysfunction. Clin Orthop Relat Res. 2010 Apr;468(4):1025-32.
Orthotics for high arches
A ‘high arched foot’ simply means that the foot’s arch is quite high creating a large area between the inside of the foot and the ground. Because there is less of your foot touching the ground, the pressure from bodyweight is spread over a smaller area. A 2005 study showed that a lot more pressure occurs under the ball and heel of the foot in a high arched foot and this pressure is significantly related to foot pain. 1 A high-arched foot is typically prone to injuries under the ball of the foot such as corns and callus, Morton’s neuroma, joint injuries and arthritis amongst others.
Orthotics for high arched feet can benefit the wearer in a number of ways. Custom orthotics for high arches are typically preferred to an orthotic purchased off- the-shelf or a ‘non-custom’ orthotic. Studies have shown that the best outcomes are achieved when orthotics are made to match the exact profile of the foot. When orthotics don’t conform to the arches very well then the patient will not have as much reduction in pain. The best orthotics for high arches will spread the pressure evenly across the foot, alleviating the high-pressure areas.
“Studies have shown that the best outcomes are achieved when orthotics are made to match the exact profile of the foot. When the orthotics don’t conform to the arches very well then the patient will not have as much reduction in pain” – Chris Hope, Podiatrist
People with high-arched feet often have difficulty absorbing shock and often experience pain or discomfort when running or walking long distances. At Entire Podiatry we offer running orthotics for high arches. These orthotics help the wearer to better absorb shock, provide cushioning and address certain biomechanical faults in order to optimise their running gait.
Some people with a high arched foot tend walk and stand with the pressure on the outside of their foot. This can predispose to ankle instability and ankle sprains. Orthotics can be designed to improve the way the foot functions to reduce the chance of injuries such as ankle sprains.

Article citation:
1 Burns J, Crosbie J, Hunt A, Ouvrier R. The effect of pes cavus on foot pain and plantar pressure. Clinical Biomechanics. 2005;20(9):877-882.
Orthotics for arthritis
Arthritis is a painful and debilitating condition affecting joints across the entire body, and the feet are no exception. There are 33 joints that hold together the human foot and any of these joints can experience arthritis.
Whilst there is yet to be a ‘cure’ for arthritis, the focus of arthritic management is on pain relief and maintaining mobility. There is evidence to support orthotic intervention as a useful conservative approach to managing both rheumatoid and osteoarthritis of the lower limbs and feet.
Orthotics for arthritis in feet
Orthotics can reduce the pain of arthritis by supporting and realigning the joints and may even slow down the progression of arthritic degeneration.
Orthotics for arthritis in the big toe and bunion pain
The big toe the most common joint in the foot to develop arthritis. Arthritis degrades the cartilage from the surface of the joints and this causes pain and inflammation. Bony spurs, known as osteophytes, also develop around the joint which causes the joint to become thickened and the movement to become restricted. Arthritis in the big toe may also exist with a bunion. A bunion or ‘hallux abductovalgus’ is a joint deformity where the big toe deviates towards the second toe and the joint becomes enlarged.
Arthritis and bunions at the big toe can have effects higher up the body. For example, with a painful arthritic big toe people often subconsciously walk on the outside of their feet to avoid moving the joint. Or they may overuse their ankles and knees to avoid bending the affected joint. Changing our walking gait to avoid pain is known as compensation, and it frequently leads to pain and overuse injuries elsewhere in the body.
Do orthotics help bunions?
It is important to note that once a bunion has developed then the only way of ‘fixing’ or ‘straightening’ the toe is through surgical correction. However there are other treatment options available to slow the rate of the bunion progression and to control the pain.
A pair of bunion orthotics may be beneficial in delaying the progression or reducing the onset of bunions or arthritis in the big toe. To ensure successful bunion treatment with orthotics, the patient’s whole foot must be considered. The best orthotics for bunions will be designed based on your individual biomechanics and taking into consideration the extent of your bunion and arthritis.
Foot orthotics for bunions can be designed in such a way to reduce the pressure on the painful joint by closely supporting the arch. Bunions often occur in those with flat feet, as the inside part of the foot at the big toe is overloaded. Orthotics for bunions and flat feet will support the arch and improve the function of the big toe.
Studies have shown that the bone just before the big toe, the first metatarsal, carries less pressure when it sits in a lower position compared to the rest of the metatarsals. If custom orthotics for bunions are designed and manufactured in a way that reduces pressure in the big toe joint this can help prevent arthritis in the big toe joint, hallux limitus, bunions and hammertoes. 1,2. Depending on the extent of the arthritis the orthotics can be designed in a way to reduce the movement at the big toe during walking to essentially immobilise the joint to provide pain relief.
Article citations:
1 Scherer P, Sanders J, Eldredge D, Duffy S, Lee R. Effect of Functional Foot Orthoses on First Metatarsophalangeal Joint Dorsiflexion in Stance and Gait. Journal of the American Podiatric Medical Association. 2006;96(6):474-481.
2 Roukis TS, Scherer PR, Anderson CF. Position of the first ray and motion of the first metatarsophalangeal joint. J Am Podiatr Med Assoc 86:538-546, 1996.
Midfoot arthritis orthotics and pain on the top of the foot
Midfoot arthritis affects the top of the foot between the front of the ankle and the toes. The midfoot is a less common location to experience arthritis but is still prevalent. Midfoot arthritis often occurs secondary to an injury or trauma to this part of the foot, such as a fracture. Arthritis may also develop secondary to abnormally high stresses to this part of the foot. For example if you have a very high arch, a lot of stress and pressure is placed at this part of the foot. There is also evidence to suggest that longstanding high-heel use may also increase the risk of developing midfoot arthritis.
An orthotic may provide relief to suffers of midfoot arthritis by supporting the arch of the foot and stabilising the midfoot. This stabilisation reduces the forces going through the midfoot and effectively works to immobilise the midfoot reducing the pain.
A study in 2009 showed symptomatic improvement in patients with midfoot arthritis treated with an orthotic 1. Another study in 2015 showed wearing custom orthotics over 12 weeks provided some benefit in treating painful midfoot arthritis 2 . This suggests that an orthotic is a viable alternative in the conservative management of patients with midfoot arthritis.
Dorsal Compression Syndrome
Dorsal Midfoot Interossseus Compression Syndrome (DMICS) is a condition whereby the ligaments along the top of the foot (the dorsal foot) are inflamed. This causes pain across the top of the foot.
DMICS is caused by too much force through the joints along the top of the foot. Any factor that causes flattening of the arches of the feet can increase these compressive forces. For example, low heeled shoes, a tight Achilles tendon and increased body weight can all contribute to the development of DMICS.
Treatment for DMICS typically involves reducing the pain and inflammation through the use of ice and anti-inflammatories. Stretching and strengthening may also be prescribed to address any problems that may be present here.
Long-term management of DMICS is generally best achieved through the use of orthotics which support the entire length of the foot. By supporting the foot, the arch is lifted and stabilised which reduced the strain through the joints on the top of the foot.

Article citations:
1 Rao S, Baumhauer J, Becica L, Nawoczenski D. Shoe Inserts Alter Plantar Loading and Function in Patients With Midfoot Arthritis. Journal of Orthopaedic & Sports Physical Therapy. 2009;39(7):522-531.
2 Halstead J, Chapman G, Gray J, Grainger A, Brown S, Wilkins R et al. Foot orthoses in the treatment of symptomatic midfoot osteoarthritis using clinical and biomechanical outcomes: a randomised feasibility study. Clinical Rheumatology. 2015;35(4):987-996.
Orthotics for knee arthritis
One third of the older adult population suffers from osteoarthritis of the knee. In an osteoarthritic knee, the cartilage that cushions and protects the bones wears away. A lack of cartilage causes the bones to essentially rub against each other, which is painful. The cartilage will wear away faster if there is a malalignment in the compartments of the knee. If there is more compression and pressure within a particular part of the joint there can be more deterioration.
This alignment can be addressed and minimised with the use of a foot orthotic 1,2. Correctly designed orthotics for knee osteoarthritis can change the position of the shin bone (the tibia) which can correct and alter the position of the knee to reduce the malalignment and reduce the pain. Evidence suggests that the earlier this orthotic intervention is begun the more effective it is.
Article citations:
1 Parkes M, Maricar N, Lunt M, LaValley M, Jones R, Segal N et al. Lateral Wedge Insoles as a Conservative Treatment for Pain in Patients With Medial Knee Osteoarthritis. JAMA. 2013;310(7):722.
2 Raja K, Dewan N. Efficacy of Knee Braces and Foot Orthoses in Conservative Management of Knee Osteoarthritis. American Journal of Physical Medicine & Rehabilitation. 2011;90(3):247-262.
Orthotics for rheumatoid arthritis
Custom foot orthotics may be helpful for patients suffering from rheumatoid arthritis. Foot pain is very common in patients with rheumatoid arthritis, with over 85% of rheumatoid sufferers experiencing pain in the feet or ankles.
Rheumatoid arthritis causes the feet to undergo considerable changes including inflammation, swelling and changes to the bone and joint position. This leads to ‘foot deformities’ where painful prominences develop such as bunions, hammertoes, claw toes, joint erosions and even dislocations. These ‘deformities’ result in areas of increased pressure beneath the foot. These high-pressure areas can lead to further problems such as corns and callus formation and skin break-down leading to a foot ulcer.
The goal of custom foot orthotics for patients with rheumatoid arthritis is to support, cushion and accommodate any ‘foot deformities’ that may be present. This helps to relieve the pain, reduce the pressure and minimise further damage from pressure overload. Due to the inflammation of the structures beneath the rheumatic foot, patients often benefit from a soft cushioned material over the orthotic to improve comfort.
Rheumatoid arthritis can also affect the ankle joint and the subtalar joint. If the ankle and subtalar joints are arthritic it can affect the patients ‘biomechanics’. An arthritic subtalar or ankle joint can significantly alter the position of the ankle and the foot, and will change the way that the feet move and function. Subtalar arthritis orthotics can stabilise the foot and the ankle in order to reduce these deformities and improve pain and restore appropriate function.
Foot orthotics for cerebral palsy
Foot orthotics, or ankle-foot orthotics (AFO) may be beneficial to patients with cerebral palsy. Standard foot orthotics provide support from underneath the foot to assist in stabilising the arch and heel. A pair of ankle-foot orthotics are similar to a regular orthotic but extend higher up the ankle and leg to increase the stability and control higher up the body.
Ankle foot orthotics for cerebral palsy can assist the wearer in improving gross motor skills such as walking, running and jumping in a number of ways.
Cerebral palsy may present with joint deformities at the feet and ankles such as contracture of the Achilles tendon and other muscular imbalances. This can be accommodated for with a pair of ankle-foot orthoses. AFOs can assist in improving the alignment of the foot and ankle. This can optimise and encourage a more balanced muscle function.
Patients with cerebral palsy often have difficulty in ensuring their feet clear the ground when walking. This can lead to frequent trips and falls. AFOs assist in achieving better ground clearance as well as encouraging a more efficient gait pattern to stabilise the centre of gravity and reduce energy expenditure when walking.
Foot orthotics may also assist in improving balance by proving a stable base of support and increasing the sensory input.
Cerebral palsy orthotics are highly specialised and individualised and an appropriate assessment will be required to ensure an appropriate device is designed to optimise the patient’s function.
Orthotics and hip pain
There are many different causes of pain in the hip including arthritis, a muscle or ligament strain, tendonitis, bursitis, a fracture or a cartilage tear. Some of these conditions can develop due to misalignment of the hip. This misalignment may be the result of poor foot posture and its associated carry-on effects higher up the body.
Often, treatment of hip pain is most effective when the entire body is considered, including an assessment from the ground up to ensure a holistic approach, rather than addressing purely the inflamed or injured tissue. Figuring out how and why the hip has been overloaded will ensure the cause of the problem is addressed, rather than just the symptoms. For example, over-pronation which is excessive ‘rolling in’ or flattening of the feet causes an internal rotation of the tibia and leg, instability around the knee and altered position of the hip. This altered position of the hip may be a contributing cause of your hip pain.
If your foot posture is deemed to be contributing to the poor mechanics and alignment of your hip then a pair of orthotics can help your hip pain. Orthotics for hip pain will be individually designed in order to reduce the strain from the affected tissue.
Can orthotics cause hip pain?
A correctly designed pair of custom foot orthotics should not cause hip pain. A new pair of orthotics can take some time to get used to as the body adjusts to the new alignment and the joints and muscles begin to work in a different way. Whilst orthotics should ultimately improve structure and function in the long term, some people may experience some discomfort during the first days or weeks of wear. If this occurs it is important that you speak to your podiatrist.
If you are wearing a pair of orthotics that are not customised, for example a pair purchased from a store or a chemist or orthotics that were not designed for you, then there is a possibility that they are not working in the correct way and they could potentially be causing pain higher up the body.
Hip pain and leg length discrepancy
A common cause of hip and lower back pain is a leg length discrepancy. This means that one leg is shorter or longer than the other.
This can be a condition that one is born with where the bones are different lengths. Or it can be the result of asymmetrical muscle tightness or strength around the gluteals, hips and lower back. This can pull and misalign the lower back, pelvis or hips causing one leg to function as a longer/shorter leg. It’s not uncommon for a leg length difference to occur after surgery, for example following a hip or knee replacement.
A leg length difference can cause uneven loading of the joints and facets of the hips, knees and lower back which can create pain and can increase the likelihood of arthritis developing. A leg length difference often changes the way that you walk and move so the body must then ‘compensate’ i.e. find a different (and often less effective) way of moving, and this compensation is often the cause of the pain.
A CT scanogram can reveal the exact length of the legs to determine the precise difference in length. Often, a professional is able to assess this without the use of CT scans, simply by measuring the legs and assessing the position of the hips and pelvis.
If your pain is deemed to be resulting from a leg length difference then foot insoles, either in the form of orthotics or a raise added to the shoes can be very beneficial to ‘balance out’ this leg difference. This, in turn, can encourage a better walking and movement pattern and can prevent any abnormal compensation by the body which is often the source of pain.
There has not been much evidence published about the use of orthotics to treat hip pain. However, at Entire Podiatry, we have found from clinical experience that many patients do respond very well to orthotics to treat hip pain.
Orthotics for lower back pain
Can orthotics help with back pain?
Lower back pain can be the result of poor alignment throughout the body. It is not uncommon to find that people who experience back pain also have abnormal gait or foot asymmetry. Abnormal biomechanics of the feet can lead to pain in other parts of the body, including the knees, hips and lower back.
For example, if your feet roll in excessively (flat feet) or if there is asymmetry between your right and left feet, then these factors can affect your posture and contribute to back pain. Back pain can also be associated with a Leg Length Discrepancy (LLD) where one leg is shorter than the other. A leg length discrepancy can change the position and alignment of the lower back and the hips and can change the way that the muscles and joints work and move. This is often a cause of lower back pain.
How do orthotics work for lower back pain?
In some cases, a pair of orthotics can help to realign the feet and legs, which can help to reduce the pain in the lower back.
“A more recent study found that those participants wearing custom-made orthotics had twice the improvement in lower back pain and for twice as long compared with the subjects using traditional lower-back pain treatments”
A podiatrist will be able to assess your foot function to determine whether your feet may be contributing to your back pain. This will involve an initial examination including history of symptoms, biomechanical assessment and gait evaluation. In order to confirm whether your foot function is contributing to back pain, we may use temporary measures (such as taping or temporary full length raises) to test whether this helps to reduce your back pain.
Following an assessment, if your podiatrist does not think your back pain is related to foot function then we will endeavour to refer you to another health care professional who will be able to assist further with your specific problem.
If your foot function is deemed to be playing a role in your back pain, then your podiatrist can offer treatment to correct the biomechanical function of your feet and legs. In many cases of back pain associated with foot function, custom foot orthotics is the most effective treatment to improve foot function. Orthotics for back pain are designed to limit any excessive motion of the feet, and to improve symmetry between the left and right feet.
The best orthotics for back pain are custom orthotics because they are designed to fit your feet exactly and are designed in a specific way to improve your alignment and function.
Multiple research studies have shown that custom foot orthotics are useful in the treatment of lower back pain. A study in 1999 found that patients with chronic lower back pain who wore custom foot orthotics had a greater improvement in their outcomes compared to those who did not wear custom foot orthotics 1. A more recent study found that those participants wearing custom-made orthotics had a twice the improvement in lower back pain and for twice as long compared with the subjects using traditional lower-back pain treatments 2.
Article citation:
1 Dananberg H, Guiliano M. Chronic low-back pain and its response to custom-made foot orthoses. Journal of the American Podiatric Medical Association. 1999;89(3):109-117.
2 Ferrari R. Effect of Customized Foot Orthotics in Addition to Usual Care for the Management of Chronic Low Back Pain Following Work-Related Low Back Injury. Journal of Manipulative and Physiological Therapeutics. 2013;36(6):359-363.
Orthotics for knee pain
The knee is a complex structure consisting of three bones, the tibia, the femur and the knee cap (the patella). Between these bones is an important structure called the meniscus which protects and cushions these bones. The knee is held in place by a number of different muscles, tendons and ligaments which are all vital to proper functioning of the knee.
If you are experiencing knee pain it is important to have this pain assessed by a professional in order to correctly diagnose your problem. Once a clear diagnosis is reached a targeted treatment plan will be devised which may include a combination of exercises for strengthening certain muscles around the knee, stretching, knee braces etc.
How can orthotics help with knee pain?
There are many different causes of knee pain and often the pain can be treated with a pair of foot orthotics for knee pain relief. The way that your foot functions can have a carry-on effect higher up the body and can affect your knees, hips and lower back.
Try this simple experiment to see the impact of foot position on your knees:
- Stand with your shoes off and feet flat on the ground. Notice the position of your knees.
- Roll your feet outward so that you are standing on the outside of your feet. Notice that your knees move outwards when you stand on the outside of your feet.
- Then try rolling your feet in. Notice that your knees tend to face inward again.
If your feet naturally tend to roll in or out too much, this places increased stress on the knee and can cause knee pain. People with high arched feet may also have knee pain, due to the feet not absorbing shock very well during gait.
Foot orthotics for knee pain work by controlling and improving your foot function which in turn improves the position and function of the knee.
Orthotics for medial knee osteoarthritis (OA)
Knee OA is a very prevalent condition and affects one third of the older adult population. There are many contributing factors to the development of OA in the knee including obesity, previous knee injury, working in a job that involves lots of bending and carrying.
OA may affect anywhere in the knee but the medial (inside) compartment is more common. This is because there are more compressive forces within the medial (inside) compartment of the knee than the lateral (outside) compartment. The excessive force causes wear down and thinning of the cartilage which sits between the bones to protect and cushion them. This is the effect of degenerative OA where the joints are no longer protected by cartilage and the knee joint is ‘bone on bone’.
There is evidence demonstrating positive effects of orthotics for medial knee pain1. A pair of orthotics can be designed in such a way to reduce compression in the inner knee, better aligning the joint spaces, evening out the loading and reducing the pain.
“A pair of orthotics can be designed in such a way to reduce compression in the inner knee, better aligning the joint spaces, evening out the loading and reducing the pain” – Chris Hope, Podiatrist
Studies have shown that using custom orthotics can decrease discomfort and stress in the medial compartment of the knee. A study in 2005 looked at 30 subjects with medial knee osteoarthritis. The subjects were given custom foot orthotics with a 5 degree lateral wedge for a 6 week period. The study found that patients with mild to moderate medial osteoarthritis had some pain relief and 28 out of 30 patients found the orthotics were comfortable. 2
These orthotics are specialised, and standard foot orthotics can make knee pain worse. Entire Podiatry are specialists in designing orthotics for patients with medial knee arthritis. It is important that whoever makes your orthotics is a specialist in biomechanics and orthotic therapy. The orthotics must be designed only after the podiatrist has conducted a thorough ‘biomechanical’ assessment of your feet and knees as well as a gait analysis. This is why custom foot orthotics are generally the best orthotics for knee pain.
Article citations:
1 Parkes M, Maricar N, Lunt M, LaValley M, Jones R, Segal N et al. Lateral Wedge Insoles as a Conservative Treatment for Pain in Patients With Medial Knee Osteoarthritis. 2019.
2 Rubin R, Menz H. Use of Laterally Wedged Custom Foot Orthoses to Reduce Pain Associated with Medial Knee Osteoarthritis. Journal of the American Podiatric Medical Association. 2005;95(4):347-352.
Orthotics for Runner’s Knee (Patellofemoral Pain Syndrome)
The term Runner’s Knee is a broad term used to describe pain typically felt around the front of the knee and the kneecap when running.
Runner’s knee can encompass many different diagnoses, however a common cause of runner’s knee is a condition known as Patellofemoral Pain Syndrome (PFPS). PFPS is a term used to classify pain in the front of the knee and behind the patella that occurs during activities which places force through the knee.
Risk Factors that can predispose an individual to PFPS include
- Large body weight
- Incorrect footwear
- Running and jumping activities, especially on hard surfaces
- Tight muscles around the knees and hips
- Imbalance of muscle strength of the inside and outside quadriceps muscles around the knee.
Your biomechanics: E.g. the way that your feet and legs move and work.- Internal rotation of the femur/thigh. This can be referred to as a ‘squinting patella’ where the kneecaps are facing slightly inwards when standing and walking.
- Valgus position of the knee. Can also be seen as an inward collapse of the knee when standing or walking or ‘knocked-knees’
- Pronated or a ‘flat foot’. A pronated or a ‘rolled in’ foot causes the shinbone, the tibia, to rotate inwards which can pace excessive stress at the knee.
These biomechanical factors can be controlled with a pair of custom foot orthotics. For example, if over-pronation is deemed to be a risk factor for the development of your PFPS then a pair of custom foot orthoses may be beneficial for your knee pain. Orthotics that are designed to prevent excessive pronation have been found to reduce pain in PFPS. A recent study found significantly greater improvements from those participants wearing orthoses compared to those without orthotics.
A study in 2004 looked at 16 patients with patellofemoral pain syndrome, who also had flat feet, and they compared the quality of life before and after wearing orthotics. There was significant improvement of patellofemoral pain with the use of custom fitted orthotics 1.
Article citation:
1 Johnston L. Effects of Foot Orthoses on Quality of Life for Individuals With Patellofemoral Pain Syndrome. Journal of Orthopaedic and Sports Physical Therapy. 2004.
Orthotics to prevent ACL injury
The ACL, or the anterior cruciate ligament is a very important ligament responsible for holding the knee in a stable position. The ACL is very prone to injury, especially in high impact and jumping sports that involve frequent change in direction such as basketball, netball, rugby, soccer and downhill skiing. A severe injury to the ACL often requires surgery and can be career ending for high-level athletes. Therefore, prevention of this type of injury is paramount.
A study published in 2008 looked at the effect of foot orthotics in knee injuries in female basketball players 1. The study found that the group of athletes who did not wear foot orthotics were 1.7 times more likely to sustain an injury to their collateral ligament and 7.14 times more likely to sustain an injury to their ACL compared to the group wearing foot orthotics.
“The study found that the group of athletes who did not wear foot orthotics were 1.7 times more likely to sustain an injury to their collateral ligament and 7.14 times more likely to sustain an injury to their ACL compared to the group wearing foot orthotics.”
At Entire Podiatry, we are experts in all types of orthotic design and prescription and we understand the demands that different sports have on the body and how to correctly consider this when designing a pair of foot orthotics.
Article citation:
1 Jenkins W, Raedeke S, Williams D. The Relationship Between the Use of Foot Orthoses and Knee Ligament Injury in Female Collegiate Basketball Players. Journal of the American Podiatric Medical Association. 2008;98(3):207-211.
Orthotics for knock-knees
Knock knees, also known as genu valgum is a condition of the legs and knees whereby there is excessive inwards bending of the knees. When standing, a person with knock knees will have a wider gap between their feet and their knees will be closer together. It is a common presentation in children under the age of 4, and most kids should grow out of this. However if knock-knees are present into adulthood then treatment may be required. The goal of treatment is not usually to ‘straighten’ the legs and knees but rather to improve the way the forces go through the knee to reduce injury and pain.
Pronated or ‘flat feet’ can contribute to knock-knees and may worsen the condition. A pair of foot orthotics can help to improve the posture and alignment of the feet, which can improve the position of the shinbone and reduce strain from the knees. The best orthotics for knock knees are a pair which are designed after conducting a thorough assessment and gait analysis by someone with an understanding of biomechanics and how the orthotic design will affect the not only the knee but the feet, ankles and hips as well.
Orthotics for bowed legs
Bow-legs is a condition where the legs appear ‘bowed’. This means that when standing there is a wider distance between the knees and the shins than there is at the feet.
People often want to know, can orthotics help with bow legs? The answer to that will depend on a few things:
The age at which the bowed-legs are appearing is important. For example, it is normal for young infants to have bowed-legs until the age of two. If the legs are remaining bowed after this age then we recommend your child is assessed by a paediatric professional as tibial bowing can also be a sign of other more serious, although thankfully rare, conditions such as:
- Blount’s disease
- Rickets
- Paget’s disease
- Fractures or bone injury
- Poisoning
In the adult population, the goal of foot orthotics for bow legs is not to “straighten” the legs and knees but rather to assist in reducing pain and improving function. Bowlegs can cause pain in the hip, knees and ankles due to the incorrect alignment of the tibia. Knee arthritis is very common in patients with bowlegs as there is more force going through the inner compartment of the knee. Knee arthritis can be a debilitating condition and this deformity can bring the onset of knee OA much earlier in life.
Bow-legs can also lead to instability around the ankles which can cause frequent ankle sprains.
Orthotics can assist in improving the alignment and forces going through the legs by improving and supporting the position of the foot. The effects of this can indirectly improve the alignment and pain further up the body to the ankles, legs, knees and hips.
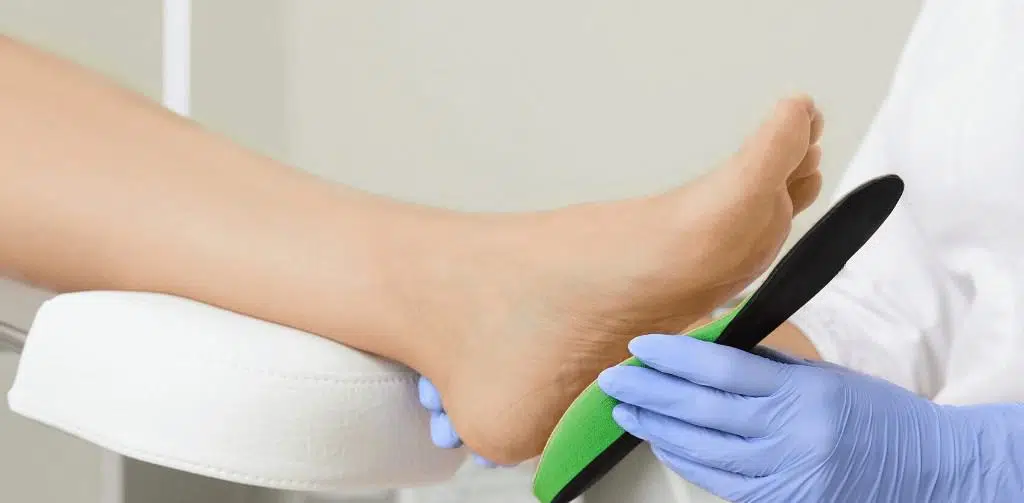
Orthotics for ankle instability/ankle sprains
Some people are susceptible to recurrent ankle sprains. This is known as chronic ankle instability. This may be due to:
- Hypermobility or excessive flexibility of the joints in the foot
- A ‘cavus’ or high arched foot
- Following a previous ankle injury. An injury may weaken the ligaments and tendons that support and stabilise the ankle joint.
Following an ankle sprain, pain and swelling can remain around the outside of the ankle and the outside of the foot. Orthotics, specifically lateral heel wedge orthotics, can be a very useful way to support the foot and reduce the chance of more ankle sprains as well as allowing healing of injuries.
A study in 2004 found an increase in ankle stability from wearing custom orthotics1. Correctly prescribed orthotics should:
- Increase sensory input from the bottom of the foot. This allows your brain to better understand the position of your foot.
- Reduce the strain from the muscles and tendons that support the ankle
- Improve the range of motion available at the ankle.
A common biomechanical presentation is a ‘cavus’ or high arched foot. In this foot the pressure is carried more on the outside of the foot. This causes the muscles, tendons and ligaments on the outside of the leg to be overused. This overuse often leads to injury and tendinopathy. Orthotics for lateral foot pain are designed to reduce the strain on these muscles and tendons on the outside of the foot. These have become known as lateral column overload orthotics. These orthotics will spread the pressure evenly across the whole foot, reducing the chance of ankle sprains and injuring the structures on the outside of the foot, ankle and leg.
If you have injured just the one ankle, we still recommend a pair of bilateral orthotics i.e. orthotics for both feet to ensure your biomechanics are corrected and addressed on both sides of your body.
Article citation:
1 Richie D. Effects of Foot Orthoses on Patients with Chronic Ankle Instability. Journal of the American Podiatric Medical Association. 2007;97(1):19-30.
Orthotics for ball of foot pain
Pain in the ball of the foot is a common presentation to podiatrists. The ball of the foot is a complex area with many different tissues that can get injured.
Orthotics are a fantastic way to address your forefoot pain. A pair of custom foot orthotics allow the podiatrist the design the orthotics in a very individualised way to address your forefoot pain. Research has shown that orthotics with good arch support and contour reduces the pressure that is carried beneath the ball of the foot, which can reduce the chance of injury occurring here1.
Ball of foot orthotics typically tend to be quite cushioned and have good arch support to spread the pressure evenly across the foot. Depending on the particular diagnoses of your forefoot pain, the part of the orthotic under the ball of your foot will be customised to address this. For example orthotics for neuroma pain will typically include a metatarsal dome. This is a small circular area of support that sits under the ball of your foot to support and lift the arch that runs across the front of your foot to open up the spaces between the bones to prevent this neuroma from being pinched and irritated. A study in 2005 showed that custom foot orthotics provided a reduction in pain for Morton’s neuroma in 63% of patients 2.

Article citation:
1 Mueller M. Efficacy and Mechanism of Orthotic Devices to Unload Metatarsal Heads in People With Diabetes and a History of Plantar Ulcers. Physical Therapy. 2016.
2 B Saygi, “Morton neuroma: comparative results of two conservative methods,” Foot & Ankle International, 26(7) (July 2005): 556-9.
Foot orthotics for plantar fasciitis
Plantar fasciitis is a common condition that causes pain beneath the heel or the arch of the foot. The plantar fascia is the name given to the main ligament under our foot which essentially creates our arch. When this ligament is over-worked then it starts to become painful either along the body of the ligament or where it attaches to the heel bone.
Plantar fasciitis usually develops because there is more strain going through the ligament than it can tolerate. There are many different treatment options available for plantar fasciitis.
One of the most effective treatments is a pair of foot orthotics, or sole orthotics for plantar fasciitis.
Do orthotics work for plantar fasciitis?
Yes. Studies have shown that orthotics, reduce pain and improve function in adults with plantar fasciitis with few risks or side effects 1,2,3. Used alone or in addition to conventional therapy (anti-inflammatory medication, stretching and strengthening, footwear modification), orthotics are effective and well tolerated by patients for short-term pain relief and improved function1,2,3.
There is no one single ‘cure’ for plantar fasciitis, rather the most effective treatment comes from the combination of changes to footwear, rest, specific exercises and stretches and adequate arch support.
There are a number of different ways that you can support your arch, including changing to more supportive footwear, strapping your foot, purchasing over the counter orthotics for plantar fasciitis or custom orthotics for plantar fasciitis from a podiatrist. Generally, customised innersoles provide the most accurate and appropriate amount of support for your foot.
For example if you are considering a pair of orthotics for high arches and plantar fasciitis you are likely to find that there you are unable to get enough arch support from an off-the-shelf device as your arch is too high for this standard fit. In this case, we recommend you consider a customised device that will provide you with sufficient arch support.

Running is an activity that puts a lot of stress through the plantar fascia, this is why plantar fasciitis is a common presentation in runners. It is important that runners see a podiatrist for an assessment of their running shoes, as this may be contributing to the overload of the fascia. Once it is known that the running shoes are appropriate then it may be a good idea to include running orthotics for plantar fasciitis into the treatment plan. Orthotics help to support the foot and the plantar fasciitis to allow the ligament to heal up correctly and to reduce the chance of this problem occurring again.
“It is important that runners see a podiatrist for an assessment of their running shoes, as this may be contributing to the overload of the fascia” – Chris Hope, Podiatrist
In recent times there has been a significant improvement to the range of the orthotic material available, in the past there was only rigid orthotics for plantar fasciitis. However, now there is a range of other material options available. This often begs the question hard or soft orthotics for plantar fasciitis? The answer to this will depend of a number of things that your podiatrist will help you to consider and understand including:
- The activity you will be doing in the orthotics
- The footwear you will be wearing the orthotics with
- Your body weight
- Your clinical presentation
- The shape and ‘type’ of your foot
- How long you expect the orthotics to last for
- Your preferences
It is important to note that hard orthotics for plantar fasciitis will usually come with a soft and cushioned protective cover over the top of the device so there will still be a soft feel under the foot.
Where to buy orthotics for plantar fasciitis?
Non-customised or off-the-shelf orthotics can be purchased from a number of different sport stores, supermarkets or chemists. However, if you want to give your feet the best chance at recovering we strongly recommend that you make an appointment with one of our podiatrists at Entire Podiatry.
Plantar fasciitis is one of the most common foot conditions we treat.
Over the past 20 years, Entire Podiatry has helped thousands of people recover from heel pain and plantar fasciitis.
We will assess your pain, develop a clear diagnosis, provide you with a range of tailored treatment options and can happily assist you with a pair of foot orthotics should this be appropriate. Contact us today for a confidential discussion.
Article citations:
1 Lewis R, Wright P, McCarthy L. Orthotics Compared to Conventional Therapy and Other Non-Surgical Treatments for Plantar Fasciitis. J Okla State Med Assoc. 2015 Dec; 108(12): 596–598.
2 Drake M, Bittenbender C, Boyles R. The Short-Term Effects of Treating Plantar Fasciitis With a Temporary Custom Foot Orthosis and Stretching. Journal of Orthopaedic & Sports Physical Therapy. 2011;41(4):221-231.
3 Whittaker G, Munteanu S, Menz H, Tan J, Rabusin C, Landorf K. Foot orthoses for plantar heel pain: a systematic review and meta-analysis. British Journal of Sports Medicine. 2017;52(5):322-328.




